Activate Data and Unlock Innovation
With powerful data management tools of the Best in KLAS data & analytics platform to accelerate your transformation
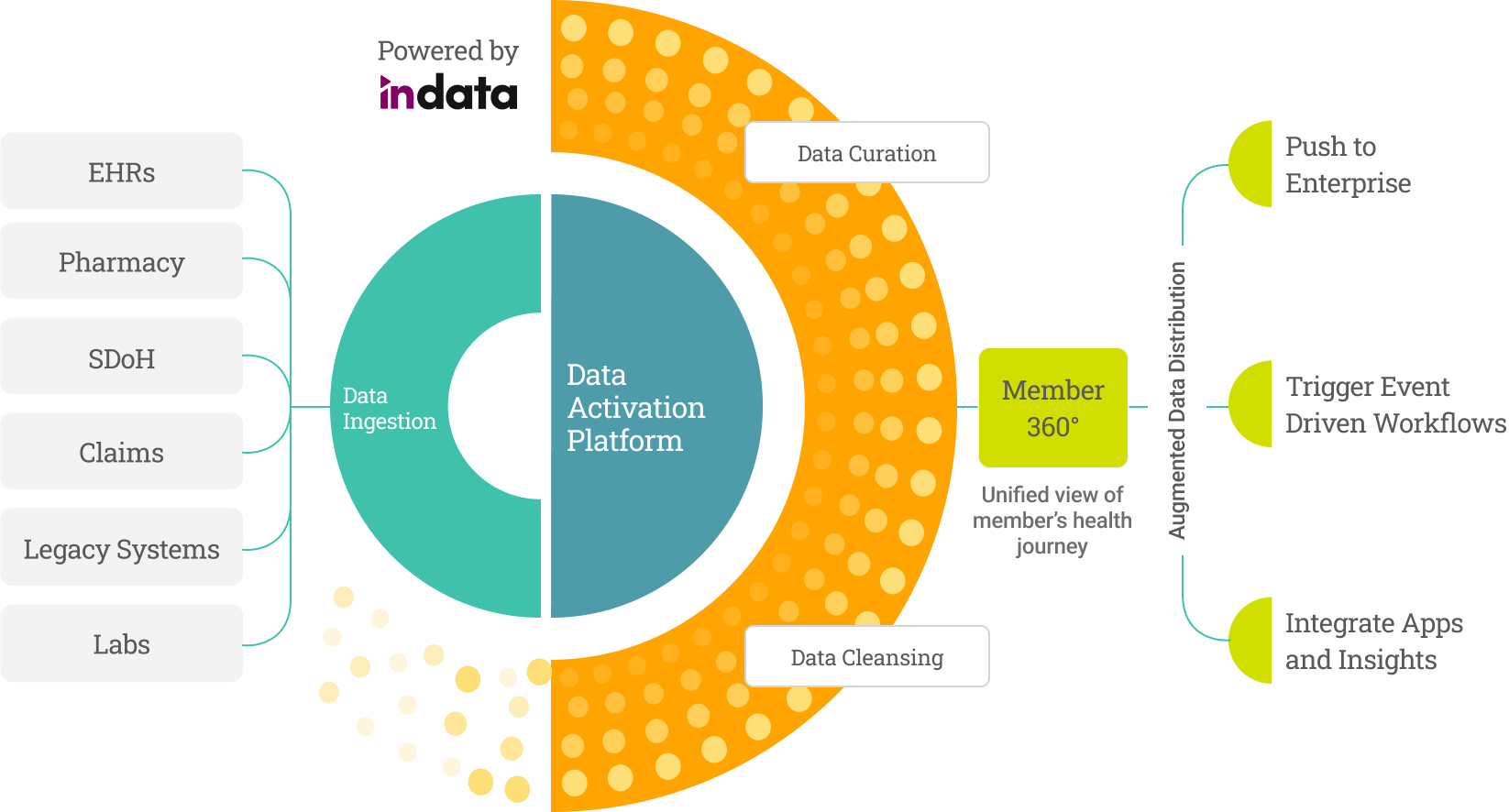
Ingest, Augment, and Distribute Activated Healthcare Data
With the industry-leading cloud-native, modular suite of data management solutions to deploy and rapidly accelerate your data transformation
Customer Stories
Request a Demo
Accelerate Your Digital Transformation with the Innovaccer Health Cloud
Request a free demo of the #1 healthcare data platform to see how you can improve care quality, patient experiences, and financial outcomes, just like our superhero customers.
/1673595227122/file.png)